Health Editor’s Note: The condition of spina bifida is when there is an incomplete development of the brain, spinal cord, or the coverings (meninges) of the brain and spinal cord. This is the most common neural tube (when the spinal cord and brain develops in the embryo) disorder and affects from 1,500 to 2,000 babies per year.
When the spine/brain is not in the protective covering of the body, nerve damage can result. There are four types of spina bifida with myelomeningocele being the most severe exposure of the spinal cord with the possibility of an inability to walk and to control the bladder and bowel.
How is spina bifida discovered before birth? The most common way to diagnose a fetus with spina bifida is to find elevated levels of serum alpha-fetoprotein in the mother’s blood. An ultrasound and possibly amniocentesis will further solidify the diagnosis.
The “cure” for a spina bifida condition is to place the exposed spinal cord back into the body, to ensure it is not damaged. In past decades this has not been accomplished until after birth, which subjects the baby to further harm its spinal cord. Now a fetus can be partially exposed, the defect is repaired, and the fetus is placed back into the uterus for the rest of its development until its delivery.
Providing protection of the spinal cord allows for babies to arrive without trauma to the spinal cord. The operation to repair the spina bifida (fetal surgery) before birth seems to have the best outcome with no/or the least amount of damage to the spinal cord and nerve systems it controls……Carol
Benefits of fetal surgery to repair spina bifida persist through school age
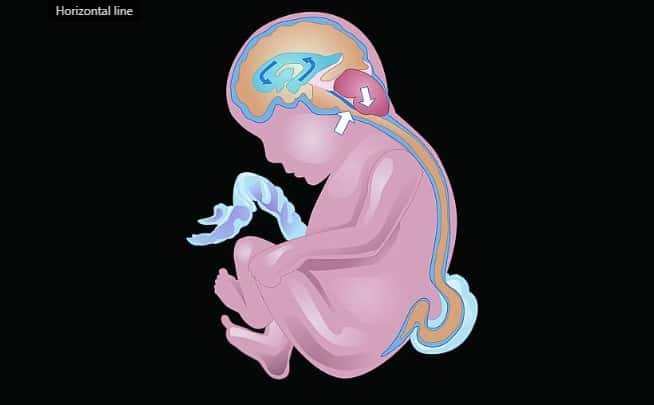
NIH.gov – With myelomeningocele, the spinal cord protrudes through an opening in the spine. The protrusion of the spinal cord may change the flow of spinal fluid and pull the brain stem into the base of the skull.
Children as young as 6 years old who underwent fetal surgery to repair a common birth defect of the spine are more likely to walk independently and have fewer follow-up surgeries, compared to those who had traditional corrective surgery after birth, according to researchers funded by the National Institutes of Health.
The procedure corrects myelomeningocele, the most serious form of spina bifida, a condition in which the spinal column fails to close around the spinal cord. With myelomeningocele, the spinal cord protrudes through an opening in the spine and may block the flow of spinal fluid and pull the brain into the base of the skull, a condition known as hindbrain herniation.
In 2011, the Management of Myelomeningocele Study, funded by NIH’s Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), found that by 12 months of age, children who had fetal surgery required fewer surgical procedures to divert, or shunt, fluid away from the brain. By 30 months, the fetal surgery group was more likely to walk without crutches or other devices.
For the current study, NICHD-funded researchers re-evaluated children from the original trial when they were 6 to 10 years old. Of the 161 children who took part in the follow-up study, 79 had been assigned to prenatal surgery and 82 had been assigned to traditional surgery. Children in the prenatal surgery group walked independently more often than those in the traditional surgery group (93% vs. 80%).
Those in the prenatal surgery group also had fewer shunt placements for hydrocephalus, or fluid buildup in the brain (49% vs. 85%), and fewer shunt replacements (47% vs. 70%). The group also scored higher on a measure of motor skills.
The two groups did not differ significantly in a test measuring communication ability, daily living skills, and social interaction skills.
“Prenatal surgery for myelomeningocele carries benefits and risks, compared to traditional postnatal surgery,” said Menachem Miodovnik, M.D., of the NICHD Pregnancy and Perinatology Branch. “This study provides important information for physicians with patients who are considering prenatal surgery.”
The study was conducted by Amy Houtrow, M.D., Ph.D., of the University of Pittsburgh, and colleagues.
About the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD): NICHD leads research and training to understand human development, improve reproductive health, enhance the lives of children and adolescents, and optimize abilities for all. For more information, visit https://www.nichd.nih.gov.
About the National Institutes of Health (NIH): NIH, the nation’s medical research agency, includes 27 Institutes and Centers and is a component of the U.S. Department of Health and Human Services. NIH is the primary federal agency conducting and supporting basic, clinical, and translational medical research, and is investigating the causes, treatments, and cures for both common and rare diseases. For more information about NIH and its programs, visit www.nih.gov.
NIH…Turning Discovery Into Health®
Reference: Houtrow AJ, et al. Prenatal repair of myelomeningocele and school-age functional outcomes. Pediatrics. 2020.

Carol graduated from Riverside White Cross School of Nursing in Columbus, Ohio and received her diploma as a registered nurse. She attended Bowling Green State University where she received a Bachelor of Arts Degree in History and Literature. She attended the University of Toledo, College of Nursing, and received a Master’s of Nursing Science Degree as an Educator.
She has traveled extensively, is a photographer, and writes on medical issues. Carol has three children RJ, Katherine, and Stephen – one daughter-in-law; Katie – two granddaughters; Isabella Marianna and Zoe Olivia – and one grandson, Alexander Paul. She also shares her life with her husband Gordon Duff, many cats, and two rescues.
ATTENTION READERS
We See The World From All Sides and Want YOU To Be Fully InformedIn fact, intentional disinformation is a disgraceful scourge in media today. So to assuage any possible errant incorrect information posted herein, we strongly encourage you to seek corroboration from other non-VT sources before forming an educated opinion.
About VT - Policies & Disclosures - Comment Policy




It’s good to know that medicine is making progress here. Everyone deserves a shot at a normal life; family, friends, passions, pastimes, discovery. Eunice Kennedy Shriver is one of my all-time heroes.
Comments are closed.